1- Introduction:
Anemia is a common complication following aneurysmal subarachnoid hemorrhage (aSAH), impacting over 50% of patients and correlating with poorer outcomes. This secondary insult can exacerbate neurological damage by further compromising cerebral oxygen delivery, potentially contributing to delayed cerebral ischemia (DCI) and other complications. While red blood cell (RBC) transfusions can augment oxygen supply to the brain, the optimal transfusion strategy in this vulnerable population has remained a subject of debate. This article provides a summary of the Subarachnoid Hemorrhage Red Cell Transfusion Strategies and Outcome (SAHARA) trial, recently published in the New England Journal of Medicine, offering insights relevant to specialists in neurocritical care and related fields.
2- The SAHARA Trial: Design and Methodology:
The SAHARA trial was a pragmatic, open-label, randomized controlled trial (RCT) conducted across 23 centers in Canada, Australia, and the United States, enrolling 742 patients. The study aimed to determine the impact of liberal versus restrictive RBC transfusion strategies on 12-month neurological outcomes in anemic aSAH patients.
- Inclusion Criteria: Adults (≥18 years) with a first-time aSAH and hemoglobin ≤10.0 g/dL within 10 days of admission.
- Exclusion Criteria: Non-aneurysmal SAH, active bleeding causing hemodynamic instability, or contraindications to blood transfusion.
- Interventions:
- Liberal Strategy: Mandatory transfusion to maintain hemoglobin >10 g/dL. This threshold was informed by physician preference, evidence of brain tissue hypoxia below this level, and data suggesting improved oxygen delivery and extraction.
- Restrictive Strategy: Transfusion only when hemoglobin ≤8 g/dL, a threshold based on specialist surveys and observational studies.
- Outcomes:
- Primary Outcome: Unfavorable neurological outcome at 12 months, defined as a modified Rankin Scale (mRS) score ≥4 (ranging from 0 [full recovery] to 6 [death]).
- Secondary Outcomes (12 months): Functional Independence Measure (FIM), EQ-5D-5L utility index and visual analogue scale (VAS), radiographic vasospasm, delayed cerebral ischemia (DCI) within 21 days, and new cerebral infarction.
- Tertiary Outcomes: Lowest daily hemoglobin (within 21 days), proportion of patients transfused, mechanical ventilation duration, ICU and hospital length of stay, and transfusion-related adverse events (within 28 days).
3- Key Findings of the SAHARA Trial:
- Primary Outcome: No statistically significant difference in unfavorable neurological outcome at 12 months between the liberal (33.5%) and restrictive (37.7%) strategies.
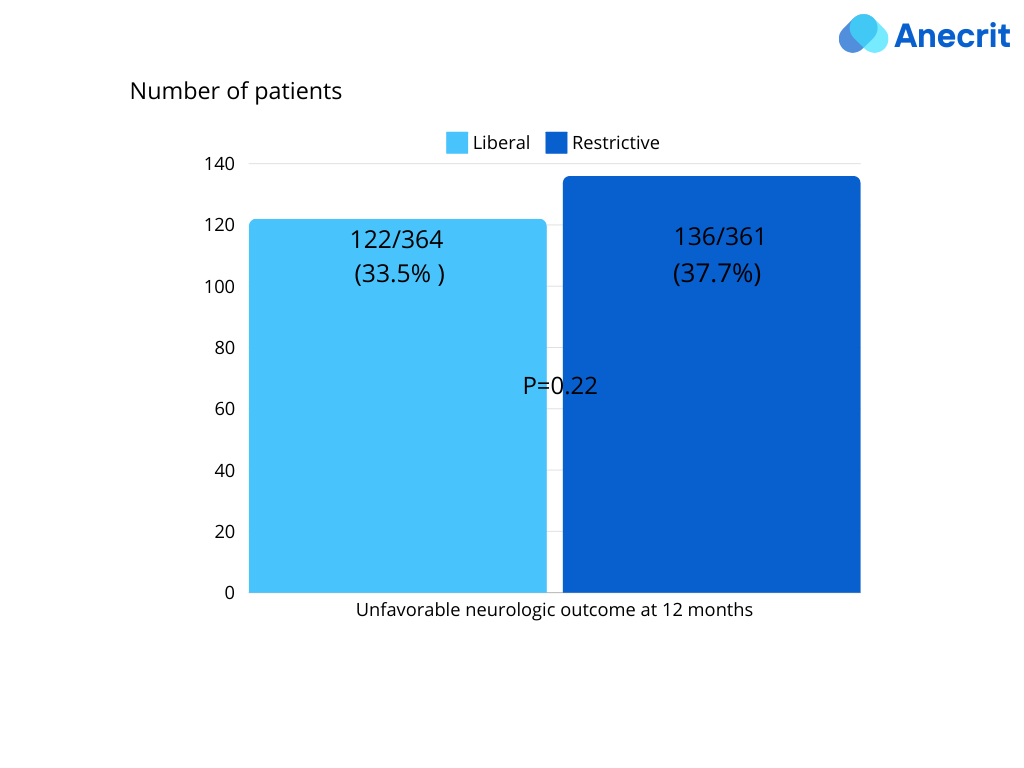
- Secondary Outcomes: No significant differences in FIM scores, EQ-5D-5L scores, VAS scores, or 12-month mortality between the groups. While radiographic vasospasm was observed more frequently in the restrictive group (40.7% vs. 31.5%), this did not translate to differences in clinical outcomes like DCI or new cerebral infarction.
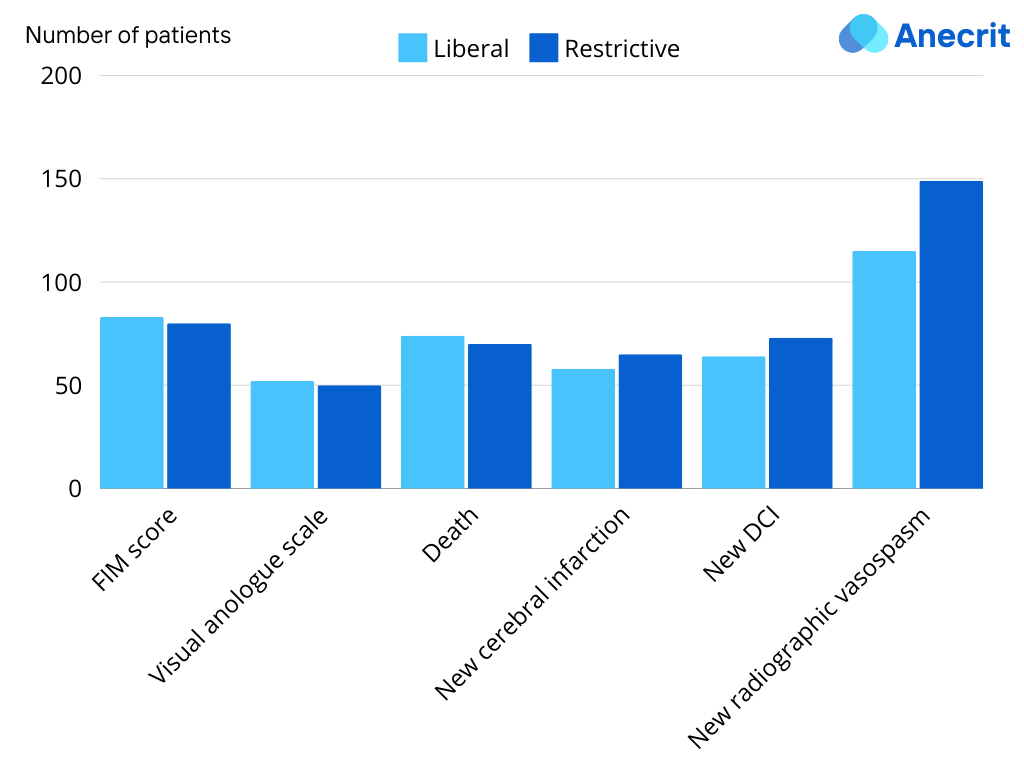
- Tertiary Outcomes: As expected, the liberal strategy resulted in significantly more transfusions (99.7% vs. 34.9%). Duration of mechanical ventilation, ICU, and hospital length of stay, and transfusion-related adverse events were similar between groups.
5- Comparison with Previous Trials:
The SAHARA trial provides crucial context when compared to other recent studies on transfusion strategies in neurocritical care, these other trials are the HEMOTION and TRAIN trials published in NEJM and JAMA respectively:
- Neurological Function Assessment: The SAHARA trial used the mRS at 12 months, whereas the HEMOTION trial and the TRAIN trial used the Glasgow Outcome Scale-Extended (GOSE) at 6 months. This difference in assessment tools and time points makes direct comparison challenging.
- Transfusion Thresholds: The HEMOTION trial in TBI patients used thresholds of ≤10 g/dL (liberal) and ≤7 g/dL (restrictive). The TRAIN trial used <9 g/dL (liberal) and <7 g/dL (restrictive). The SAHARA trial used ≤10 g/dL (liberal) and ≤8 g/dL (restrictive). These variations in thresholds highlight the ongoing debate regarding optimal hemoglobin targets.
- Patient Population: The HEMOTION trial focused on traumatic brain injury (TBI), while the TRAIN trial included a heterogeneous neurocritical care population (only 23% with SAH). SAHARA specifically targeted aSAH patients, providing more targeted data for this population.
- Results: While the HEMOTION trial, like SAHARA, found no difference between strategies, the TRAIN trial suggested a benefit of a liberal strategy in acute brain injury. This discrepancy may be due to differences in patient populations, transfusion thresholds, and outcome measures.
6- Clinical Implications:
The SAHARA trial provides robust evidence supporting the use of a restrictive transfusion strategy in anemic aSAH patients. The findings demonstrate that a restrictive approach is non-inferior to a liberal strategy in achieving favorable 12-month neurological outcomes. This has significant implications for resource utilization and minimizing unnecessary transfusion-related risks.
7- Conclusion:
The SAHARA trial represents a significant contribution to the management of aSAH. Its rigorous methodology and focused patient population offer valuable guidance for clinicians. The findings suggest that a restrictive transfusion strategy (transfusing at ≤8 g/dL) is a safe and effective approach in anemic aSAH patients, challenging previous assumptions and potentially refining clinical practice. Further research is needed to explore the optimal transfusion strategies in specific subgroups of aSAH patients and to investigate the long-term impact of these strategies on cognitive and functional outcomes.
References:
- Liberal or Restrictive Transfusion Strategy in Aneurysmal Subarachnoid Hemorrhage. N Engl J Med. 2024 Dec 9. doi: 10.1056/NEJMoa2410962. (SAHARA trial).
- Liberal or Restrictive Transfusion Strategy in Patients with Traumatic Brain Injury. N Engl J Med. 2024 Aug 22;391(8):722-735. doi: 10.1056/NEJMoa2404360. (HEMOTION trial).
- Restrictive vs Liberal Transfusion Strategy in Patients With Acute Brain Injury: The TRAIN Randomized Clinical Trial. JAMA. 2024 Nov 19;332(19):1623-1633. doi: 10.1001/jama.2024.20424. (TRAIN trial).
Keywords: aSAH, red blood cell transfusion, SAHARA trial, neurocritical care, anemia.

Comments ()